Cramps
One topic which has come up a lot with my patients lately is the issue of muscle cramps. You probably have experienced cramps yourself. You are sleeping peacefully and all of the sudden there is an extreme pain in your leg, or your back. Suddenly, you have a spasm where it becomes difficult for you to move. This can be very irritating and painful and it may take a little while for you to return to normal. Why does this happen?
I myself experienced some bad cramping after a particularly difficult workout while I was swimming. I had pushed off the wall doing several laps and that night I woke up in agony. This can occur when there has been an overuse of your muscles. My body was not used to this repeated activity. In a measure to protect itself, my body decided to contract the muscles I had overused. To put it simply, I had cramps.
What is the cause?
There can be other reasons you might develop cramps as well.
- Poor Blood Supply: Cramps can occur due to inadequate blood supply. Narrowing of your arteries can cause cramp like symptoms in your legs or feet. This usually happens when you are in motion and generally stops once you stop exercising.
- Neurogenic claudication: This is a condition which has similar symptoms as those listed above, however it is due to issues in the neurological system. Stenosis, or a narrowing of the opening where your nerves exit the spinal cord, can cause pain in your legs while you are moving and exercising. This can also mimic sciatica or radiate pain down your legs. In any case, it is very painful.
- Dehydration: Dehydration can lead to a poor balance of potassium, calcium or magnesium in your system which can also cause cramps. Some medications can deplete these minerals.
Those who are most affected by this are people with certain medical conditions such as high blood pressure, the elderly (who are prone to dehydration), athletes who do not properly hydrate during activity, or those who live in a hot climate. Pregnancy is also known to lead to uncomfortable cramps.
How Can I Stop the Cramps?
What can be done to avoid and overcome these things? Well, the most important thing is to keep yourself hydrated. Drinking plenty of liquids is essential to your health. What is the right amount? Well, that depends on your age, activity level, medical condition or the weather where you live. It is best to speak with your health care provider in order to come up with the answer. Another thing you can do is stretch your muscles which are the most prone to cramping. Your calves and your hamstrings are major offenders when it comes to cramps. There are several stretches for your calves which are good but I have one favorite. It looks like this:
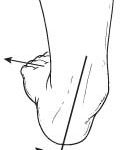
Roll up a towel and step on it, keeping it on the front 1/3 of your foot. Hold this stretch for about 30-35 seconds and do it about 3 times. This supports the plantar fascia and stretches your calves very safely. Do this after activity, or before bed if you often get cramps at night.
Always seek medical attention if your symptoms are extremely severe, or if the pain is associated with swelling, extreme tenderness, or skin changes. Also, if you have weakness that you cannot explain. If you have any questions, please see your doctor or another health care practitioner. We are happy to answer any additional questions you may have.
Post written by Rod Walker, PT