As I continue in my career as a physical therapist, one of the most common problems I treat is lower back pain. This can affect anybody, from the young to the old. There are various reasons that one can have low back pain, but most of the time there are common issues that those who are in pain share. A little information can help in order to reduce your pain.
First off, let’s review a little about your spine. Your spine is flexible and can move in different directions based on the positioning of the facet joints, the movable areas of the spine, and where those individual segments connect the bone above and below it. There are also muscles which attach directly to the bones of the spine, and those adjacent to it which can cause problems. It’s often abnormalities in these muscles that can be the cause of your back pain. Certain muscles can be weak or tight which can limit mobility. This causes pressure where there shouldn’t be, and that causes pain.
Muscles which can cause trouble: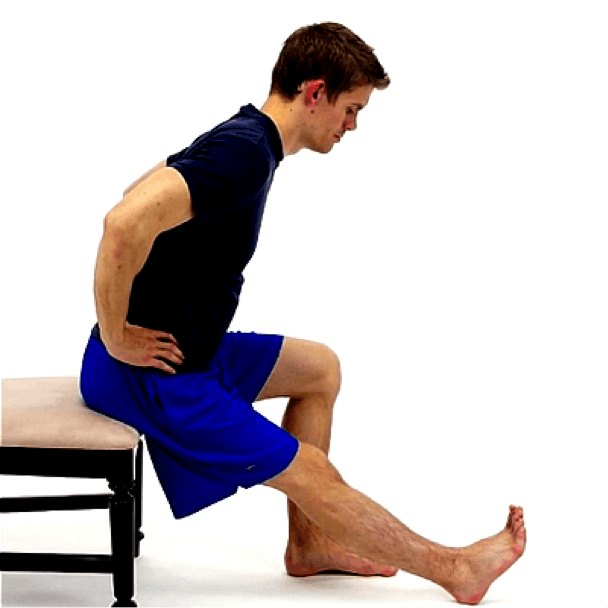
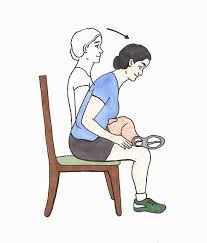
- Hamstrings: The hamstrings are a group of muscles on the back of your upper leg. If these are tight, they affect how your hip bones move. If they are really stiff they can rotate your pelvis backward, which pulls at your spine. A great way to stretch these is to sit in a chair with your leg extended in front of you, your heel on the ground, and lean forward keeping your back straight. Most people want to reach down the leg but I suggest keeping your hands at the top of your leg and supporting your straight back. Hold this for 30-45 seconds. Perform this move about 3 times, and do a set a few times per day.
- Piriformis- Next, the piriformis is a muscle that is beneath your glute muscle group. Most people know where their gluteus maximus is. Well, this muscle is right beneath it. It runs from your sacrum, which is what you sit on, to behind the big bump on the outside of your upper leg called the Greater Trochanter. An easy way to stretch this is to sit and cross the affected leg over to where your ankle is resting on your opposite knee. Your lower leg should be as flat as possible. Gently lean forward until you feel a gentle stretch in the back of your buttock. Hold this for 30-45 seconds. Do this three times in a row, a few times per day.
Stretching not Screeching
Lastly, and the most important thing about stretches is: they should not hurt! If they hurt, you’re going too far. This is so important because a stretch that hurts is typically a muscle contraction, which is a shortening of the muscle. This is the exact opposite of what we are trying to achieve, so don’t do it! Remember these two factors are just the tip of the iceberg of what can be causing your pain. If you want to get more details, please consult with a professional so you can get properly diagnosed in order to return to all of your daily activities. Happy stretching!
Post written by Rod Walker, PT